Pediatric deceased donor liver transplantation with in situ size reduction for recipient-graft size matching
Jung-Man Namgoong
1, Shin Hwang
1, Dae-Yeon Kim
1, Tae-Yong Ha
1, Gi-Won Song
1, Dong-Hwan Jung
1, Kyung Mo Kim
2, Seak Hee Oh
21
Department of Surgery, Asan Medical Center, University of Ulsan College of Medicine, Seoul, Korea,
2
Department of Pediatrics, Asan Medical Center, University of Ulsan College of Medicine, Seoul, Korea
Case Report
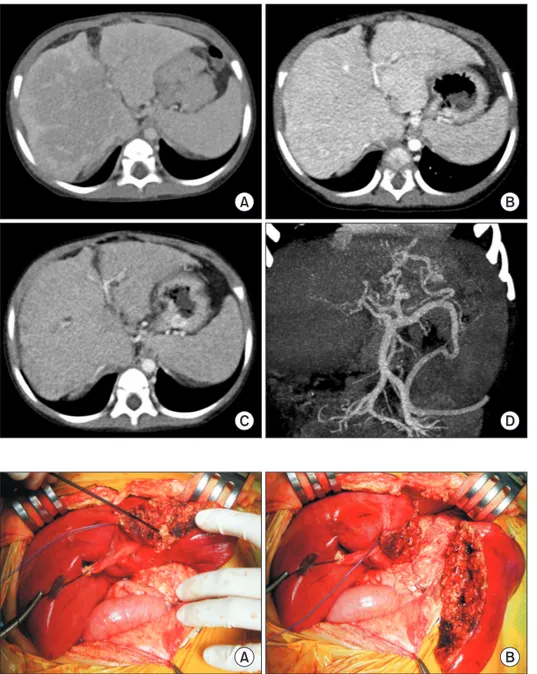
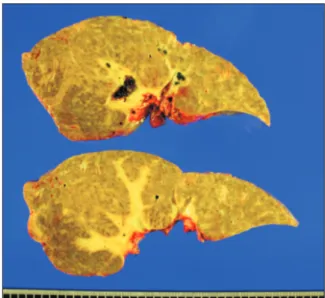
We present a case of pediatric deceased donor liver transplantation using a reduced whole liver graft in a 25-month-old boy weighing 12.7 kg. After he had undergone Kasai portoenterostomy for biliary atresia, his general condition deteriorated progressively. He was enrolled on the waiting list for liver transplantation with Pediatric End-stage Liver Disease score of 15. The donor was a 51-month- old boy with body weight of 20 kg. The donor-to-recipient body weight ratio was 158%. The liver graft appeared to be larger than the recipient’s abdominal cavity. Thus, we planned to do in situ size reduction. Recipient surgery was performed following standard proce- dures. We performed graft outflow vein reconstruction using a modified piggyback technique like the double inferior vena cava meth- od. Since the portal vein was hypoplastic, a side-to-side anastomosis technique was used. We also performed intraoperative portogram to embolize venous collaterals. After completing the graft implantation, we found that the liver graft was too large to be accommodat- ed within the abdomen. After in situ resection of the left lateral section parenchyma, we successfully performed primary closure of the abdominal wound. This patient experienced episodes of acute rejection. He has been doing well for four years after the transplanta- tion.
Key Words: Large-for-size graft; Pediatric transplantation; Graft-recipient weight ratio; Reduced graft; Left lateral section
INTRODUCTION
Liver transplantation (LT) is a life-saving procedure for chil- dren with end-stage liver disease. The success of LT is attribut- ed to the development of effective therapies for immunosup- pression and evolution of surgical techniques that have allowed many more children to receive LT [1-3]. Because most pediatric recipients are under three years of age, there is a significant shortage of size-appropriate whole organs for these patients [3].
Therefore, innovative surgical techniques have been developed to expand the procedure to a wider number of patients, includ- ing split deceased donor liver grafts, partial living donor liver
graft, reduced and hyper-reduced liver grafts, and whole liver grafts.
Living donor liver transplantation (LDLT) has been fre- quently performed because of serious deceased donor shortage in Korea. Types of pediatric LT performed are in the order of LDLT, split LT, whole liver deceased donor LT, and reduced deceased donor LT. In real-world practice in Korea, if a whole liver from an adult deceased donor is too large for an adult patient, split LT for two adult patients is preferred instead of performing reduced LT [4,5]. In contrast, if a whole liver from a pediatric deceased donor is too large for a pediatric patient, there is no practical choice other than to perform reduced LT.
Considering that the incidence of pediatric deceased donors is very low, the actual incidence of reduced LT for pediatric pa- tients is much more lower in Korea. We herein present a case of reduced LT done in a 25-month-old recipient using a liver graft from a 51-month-old deceased donor.
CASE
The recipient was a 25-month-old boy who had undergone Kasai portoenterostomy at the age of 2 months for biliary
Received: September 29, 2020, Revised: October 2, 2020, Accepted: October 3, 2020
Corresponding author: Shin Hwang
Department of Surgery, Asan Medical Center, University of Ulsan College of Medicine, 88 Olympic-ro 43-gil, Songpa-gu, Seoul 05505, Korea
Tel: +82-2-3010-3930, Fax: +82-2-3010-6701, E-mail: [email protected] ORCID: https://orcid.org/0000-0002-9045-2531
Copyright Ⓒ The Korean Association of Hepato-Biliary-Pancreatic Surgery
This is an Open Access article distributed under the terms of the Creative Commons Attri- bution Non-Commercial License (http://creativecommons.org/licenses/by-nc/4.0) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.